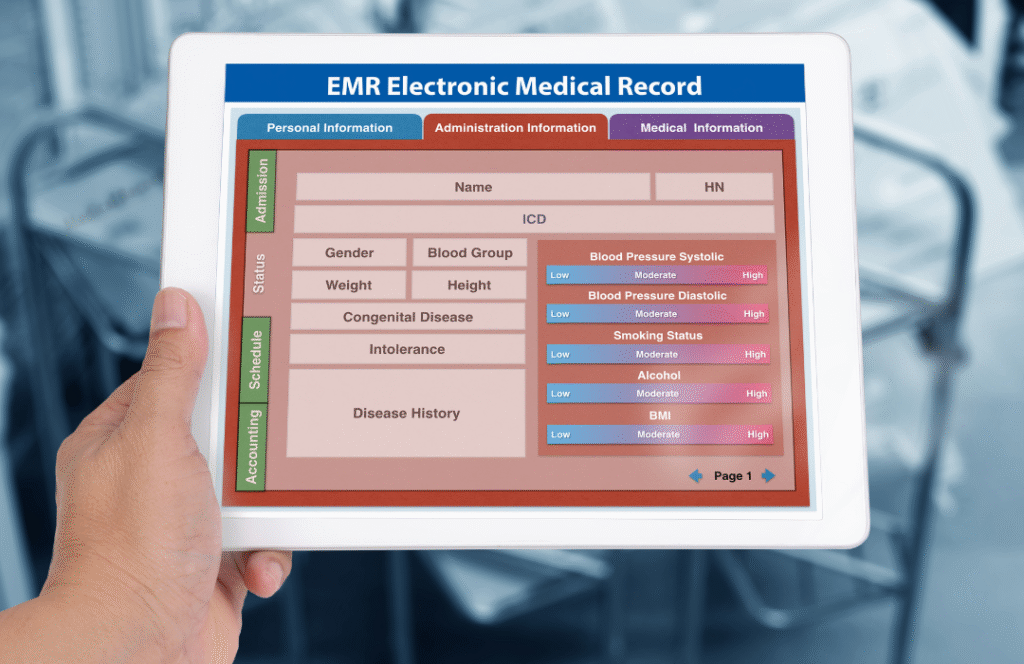
You can’t force a machine into a heartbeat.
There’s a nurse who rounds with a tablet in one hand and a patient’s trembling hand in the other. She’s trying to listen to a story about meds, allergies, and the way a child’s laugh sounds when remembering a grandfather, and the screen keeps demanding things that don’t belong in that moment. That tension is the whole problem: EMRs that don’t fit human rhythm turn care into a series of interruptions. Integration is the patient centered antidote.
The problem in one breath
EMRs were meant to weave information into care. Too often they become seams that snag: multiple clicks to record a single observation, duplicate entries in three systems, and alerts that scream without context. The result is fractured attention, stretched compassion, and time stolen from bedside moments.
Why integration is more than tech it’s choreography
Think of a hospital as an orchestra. Clinicians are musicians. Patients are the music. An integrated EMR is the conductor who knows the score and cues the right instrument at the right time. Without it, the music becomes noise.
When systems talk to each other, workflows stop being a tangle of handoffs and start being a flow:
- labs appear where they should, not where someone remembers to print them;
- medication history travels with the patient, not as a fragmented story.
- Triage, imaging, and specialty notes cascade into the chart as a single narrative, not as separate monologues.
That’s the difference between an EMR that stores data and one that serves care.
Real pain points (the human toll)
- Context switching: Clinicians juggle screens instead of holding a patient’s gaze.
- Duplicate documentation: Time spent copying data is time lost for empathy.
- Alert fatigue: Urgent tones for trivial matters erode trust in the system.
- Broken handoffs: When data doesn’t travel, families repeat trauma at every desk.
These aren’t abstract frustrations. They’re the reason a parent waits longer, why a nurse skips a break, and why a clinician dreams of simpler days.
How EMRs should adapt to human rhythm: practical, humane moves
- Map real workflows, not ideal ones.
Watch clinicians do their work. Shadow mid-shift. Document the real steps, the workarounds, and the whispered hacks. Technology must mirror real practice, not the glossy version shown in demos. - Co-design with end-users.
Put nurses, physicians, pharmacists, and receptionists at the design table. Their small fixes, which reword a prompt or remove a required field, often yield the biggest relief. - Make data move with the patient.
Seamless interoperability (the kind that respects context and ownership) prevents story loss. When a patient crosses systems, their narrative should cross with them complete and legible. - Prioritize context aware interfaces.
Show what matters now: the bedside view should surface vitals and recent meds; the clinic view surfaces chronic care plans. Same patient, different lens - Voice & natural interactions where it helps.
Voice to note and smart templates let clinicians speak the story while keeping hands available for care. But keep corrections easy and visible; the voice is an assistant, not a dictator. - Intelligent alerting, not alarm storms.
Tune thresholds, cluster related notifications, and introduce “soft alerts” that suggest rather than demand. Trust returns when alerts respect judgment. - Measure the right things.
Track minutes regained at the bedside, reduction in repeat history calls, and clinician satisfaction, not just uptime and CPU cycles. - Train, iterate, and listen forever.
Integration is continuous. Run short pilots, collect rapid feedback, fix fast, and celebrate small wins. Make super-users and clinical champions the permanent bridge between IT and care. - Design for downtime & degraded modes.
If the system fails, clinicians must still have graceful, fast paperless fallbacks portable views, sync queues, and offline modes that reconcile later. - Governance that centers care.
Create cross-discipline councils (clinicians, IT, ops, patients) that decide which workflows change and why, so upgrades don’t arrive as surprises.
A small example you can taste
Imagine an ED where the triage tablet auto-populates prior visits, allergies, and last-seen vitals. The nurse’s shorthand notes convert into a succinct history the doctor reads aloud at bedside. Orders flow to the lab automatically, and when results come, a single contextual alert arrives: “Troponin rising; consider cardiology consult.” No separate logins, no repeated questions, just a thread of care. That’s the heartbeat returning.
The quiet payoff
Integration isn’t flashy. It doesn’t look good on a slide. But it returns what matters: time at the bedside, fewer repetitive tasks, clearer handoffs, and less burnout. It turns EMRs from gatekeepers into companions systems that move with care rather than forcing clinicians to move around them.
Final thought: an invitation
You can’t force a machine into a human heartbeat. But you can design systems that learn the rhythm. Start by listening really listening to the people who do the work. Map their steps. Build from there. Because when EMRs follow the human pulse, everything else falls into place: safer decisions, kinder encounters, and a care system that finally sounds like a song instead of a clatter of keys.